Stress and Your Skin: Watch Out for These 4 Problems
Stress is one of the most persistent and destructive health challenges. In addition to raising your risk of internal health problems, stress can affect your external organ — the skin — in some unattractive and uncomfortable ways.
If you want to maintain your skin’s optimal well-being, you need to understand how stress can affect your skin, what you can do about the conditions that it might aggravate, and how to prevent chronic stress from turning into flare-ups of various conditions. Read on to learn four ways your skin may react to constant or severe stress.
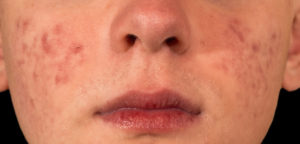
1. Acne
Teenagers commonly experience acne as the natural result of strong hormonal shifts that occur during adolescence. However, the body’s reactions to stress can also alter hormonal balances, both in adolescence and throughout adulthood. Stress makes the body release large amounts of cortisol, which increases pore-clogging oil production.
Stress-induced acne may trigger isolated breakouts during tough times, or acne may linger as a side effect of an uncontrolled chronic stress disorder. To make matters worse, stress can interfere with the body’s healing and repair processes, making it harder for your acne breakouts to resolve themselves without treatment from a dermatologist.
2. Rosacea
Rosacea can prove just as irritating and embarrassing as acne. This inflammatory condition can leave you with a red face, visible blood vessels just under the skin, and/or itchy, bumpy rashes. A variety of factors can cause or worsen rosacea outbreaks, from cold weather and excessive sunlight exposure to stress.
Medical research has confirmed the links between extreme stress and rosacea problems. 91 percent of study respondents noted that their outbreaks seemed to occur under stressful conditions, with 45 percent of them reporting more frequent rosacea outbreaks because of their stress.
The fact that many people may self-medicate their stress with alcohol only adds fuel to rosacea’s fire. Alcohol consumption causes blood vessels to dilate, allowing more blood to rush to the face and triggering bouts of rosacea.
3. Psoriasis
Just as suppressed immune function can complicate your ability to get over acne breakouts, a suppressed immune system can also make you more vulnerable to psoriasis. This autoimmune condition occurs when the skin overproduces new cells, creating scaly, discolored, itchy patches that can make you miserable.
Dermatologists typically prescribe topical corticosteroids to fight psoriasis by reducing skin inflammation, along with products containing retinoids (which discourage skin cell overgrowth), salicylic acid, or coal tar. More severe psoriasis may require treatment with biologic drugs that can tame those overactive immune responses.
4. Eczema
You might have trouble telling eczema and psoriasis apart at first glance since both conditions cause itchy, unsightly skin rashes. However, unlike psoriasis’s obvious link to autoimmune issues, eczema occurs for less clear reasons. Hot temperatures, harsh soaps, dust exposure, and stress can all induce eczema attacks.
Your dermatologist may recommend some home care practices that can ease your eczema symptoms and help you avoid recurrences. For instance, you may get relief from cool compresses, over-the-counter topical creams, and antihistamines. You might also feel better by reducing your exposure to hot weather and dust
Your dermatologist can administer stronger treatments if home care measures fail. In addition to antibiotics for patches of broken skin that get infected, you may need medications such as methotrexate, azathioprine, or dupumilab. At the same time, you may also benefit from separate treatment for an underlying chronic stress disorder.
If you suffer from any of the skin problems listed above, visit East Carolina Dermatology & Skin Surgery. Our dermatology team can examine your symptoms, discuss your medical history and lifestyle, and create a personalized plan for dealing with your condition. Contact us today for an appointment.
