4 Key Points About Solar Urticaria
As temperatures rise and sunny days grow more frequent, many people love to go outdoors and enjoy their favorite activities. Unfortunately, some individuals may find their time in the sun less than enjoyable due to a rare and irritating skin reaction known as solar urticaria.
If you experience mysterious rashes whenever you experience any degree of sun exposure, you may suffer from solar urticaria. Fortunately, you can fight back against this frustrating issue once you know more about the condition’s characteristics and management strategies. Start by absorbing the following four key points.
1. Solar Urticaria Involves an Allergic Reaction
When you think of allergies, you probably envision reactions to pollen, chemicals, foods, pet dander, and other substances that the immune system misidentifies as threats. The immune system responds to these substances by producing histamine and antibodies to attack them, creating allergy symptoms in the process.
In the case of solar urticaria, the immune system reacts abnormally to your own skin cells when those cells receive sunlight. For reasons dermatologists don’t completely understand, the sunlight causes the skin’s mast cells to set off an immune system response, resulting in an allergic reaction.
2. Solar Urticaria Causes Rash-Like Symptoms
Solar urticaria occurs more commonly on parts of your skin that are exposed to the sun, either through direct exposure or through thin clothing. Common symptoms include tiny, itchy, red bumps that may form into a larger cluster of hives. The resulting rash may also hurt, bleed, or crust.
Thankfully, most bouts of solar urticaria fade away without leaving any scars after you get out of the sun, usually within 24 hours or less. However, extreme cases of solar urticaria can cause longer-lasting symptoms, such as nausea, fatigue, breathing difficulties, or even a dangerous condition called anaphylaxis.
3. Diagnostic Testing Can Identify Solar Urticaria
You might confuse the signs of solar urticaria with those of other skin problems such as heat rashes, especially if they occur on warm, sunny days. However, solar urticaria only develops in sun-exposed skin, while a heat rash more commonly develops in areas that don’t receive sun, such as skin folds where heat and sweat accumulate.
Since solar urticaria can closely resemble other kinds of allergic reactions, you should consult a dermatologist to confirm the cause of your symptoms. Your dermatologist may diagnose solar urticaria based on your medical history and recent sun exposure. However, testing your skin’s reactions under a UV lamp can confirm the diagnosis.
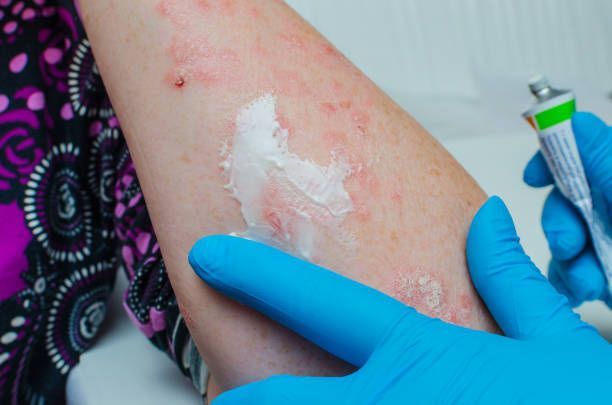
4. Treatment and Preventative Care Can Ease Solar Urticaria
Even if your solar urticaria symptoms resolve on their own, you may still experience discomfort and embarrassment during an outbreak. To ease your symptoms, your dermatologist may prescribe calamine lotion, oral antihistamines, corticosteroids, and/or an antimalarial medication called hydroxychloroquine.
If you tend to get solar urticaria in the summer, your dermatologist may also recommend that you try to desensitize your skin to sunlight during the spring months. This process involves regular sessions of exposure to an ultraviolet sun lamp. However, you might need to repeat this regimen periodically if the benefits don’t last.
You can’t necessarily hide from the sun all the time, but you can protect your skin against it. Wear UV-blocking clothes that cover as much skin as possible, along with a broad-brimmed hat and sunscreen that protects exposed skin from UV radiation. You can also try to avoid exposure by remaining indoors during peak sun hours.
If your skin responds to sun exposure in a manner that suggests solar urticaria, get the professional evaluation and treatment you need at East Carolina Dermatology and Skin Surgery. Our dermatology team can pinpoint the underlying cause of your symptoms and help you manage the problem. Contact us today.